During your consultation, your surgeon will walk you through the three main decisions(1):
- Which implants are recommended for your needs >>
- The implants’ positioning >> and
- Where to perform the surgery incision
In this article we will focus on the latter and explain the main areas where your breast surgery incisions can be made.
What is the purpose of the surgery incision?
In order to insert the breast implant, your surgeon will have to make an incision, usually in one of the following locations: the crease under your breast (inframammary fold incision), under your arm (transaxillary incision), or along the border of the areola (periareolar incision).
Other less popular options are through the umbilicus, or belly button, and through the upper margin of an abdominoplasty flap(1). Since these options are not widely used, we will explain the three common incision options as well as their benefits and limitations.
The incisions (and the surgical scar that remains) are one of the most common concerns for patients. In breast augmentation surgeries they are indeed necessary but can be usually concealed.
Inframmary incision
The inframammary incision was the original approach for breast implant insertion (1) and it remains the most popular nowadays(5,6,9).
This incision is made in the natural crease of the breast (as shown in the image below) and it provides the surgeon with a direct route of insertion, great visibility, and ability to expand the incision when necessary(1).
This incision can be used to achieve all breast implant positions and allows the insertion of a highly cohesive silicone gel implant(1).
The main drawback of this incision is the location of the incision itself, which might be slightly more visible than those made under the arm or around the areola. However, plastic and cosmetic surgeons are skilled in making incisions less visible.
The lower interference with breastfeeding (8), make this incision a popular choice for surgeons and patients alike, despite the slightly larger incision size.

Transaxillary or axillary incision
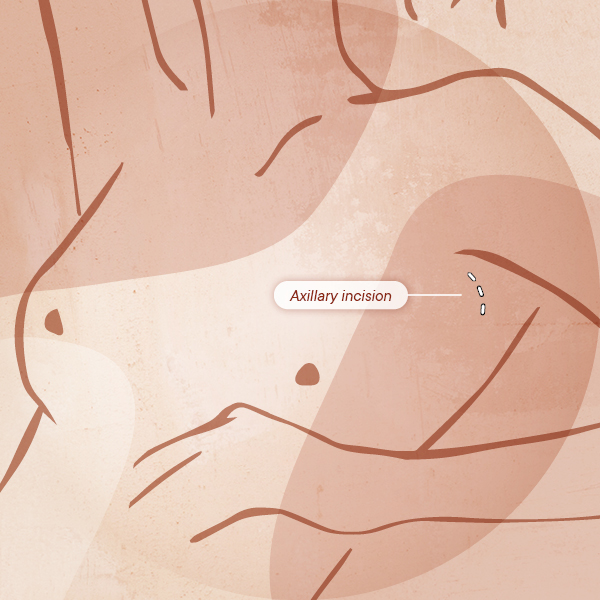
The axillary incision was developed in the 1970s(1,4) and it is a well-known technique(2). It consists of an incision made under the arm (as shown in the image below).
This incision can be made to achieve different breast implant positions and it has the main advantage of minimally visible scars(2).
As with the inframammary incision, this incision is also a good option if you wish to nurse in the future, since it has a lower probability of complications with breastfeeding(8).
The transaxillary incision has some limitations, such as limited implant choice, less control in implant positioning, possible nerve and lymphatic damage in the axilla and potential muscular distortion(2,10). Disadvantages might also arise years after the surgery is completed.
When the incision is located in a remote region such as the axilla, secondary procedures and implant replacement may be difficult; therefore, an additional inframammary incision may be necessary. In this case, the previous axillary approach's aesthetic benefit could be lost(2, 10).
An important aspect to consider is that pathologic analysis of axillary lymph nodes provides crucial information for adjuvant therapies used to manage breast cancer. The axillary incision does not necessarily affect lymph nodes, but it can, so this factor needs to be considered when choosing this approach(2).
Periareolar incision
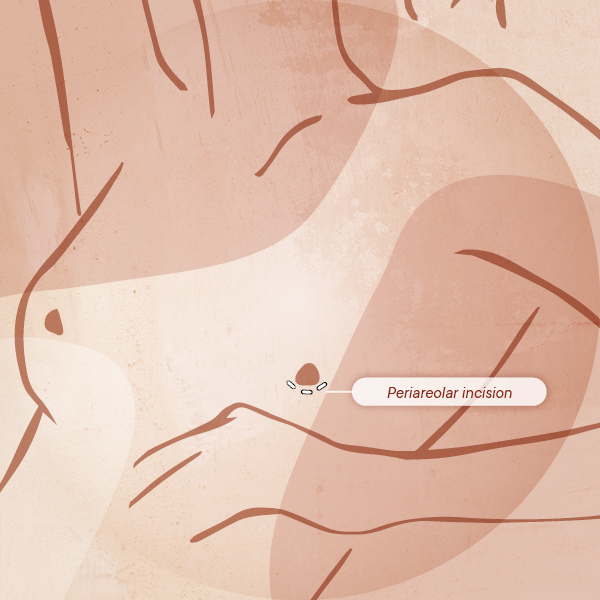
The periareolar incision consists of an incision made around the areola (as shown in the image below) and, thanks to skin pigmentation, it can result in an almost indistinct scar(1).
This incision can be used to achieve all breast implant positions(14).
Limitations include the inability to expand the incision if necessary(1), possible loss of nipple sensitivity(3,7), hyperpigmentation in the areola(3), high rates of capsular contracture(13) and the highest risk of surgical site infection(1).
Although the periareolar incision is closer to the nipple and areola than other incisions, it technically does not increase the risk of breastfeeding problems after surgery(8, 9). However, the risk cannot be completely eliminated. If you wish to breastfeed in the future, share your intentions with your surgeon, so she or he can take this factor into account when choosing the incision site(7).
How to make a decision
The best incision for you will depend on your personal needs and anatomy.
As explained in this article, there are pros and cons to each type of breast implant incision, but everyone has a different idea of what is most important to them. You will be able to discuss the different options with your surgeon in order to make a decision.
To better understand your procedure, we also encourage you to read our previous articles around implant selection and implant placement. Write down all your questions and don’t forget to cross-check all the information with your surgeon!
SOURCES:
(1) Pelosi, M. A., & Pelosi, M. A. (2010). Breast Augmentation. Obstetrics and Gynecology Clinics of North America, 37(4), 533–546. https://doi.org/10.1016/J.OGC.2010.09.003
(2) Munhoz, A. M., Fells, K., Arruda, E., Montag, E., Okada, A., Aldrighi, C., … Ferreira, M. C. (2006). Subfascial Transaxillary Breast Augmentation Without Endoscopic Assistance: Technical Aspects and Outcome. Aesthetic Plastic Surgery, 30(5), 503–512. https://doi.org/10.1007/S00266-006-0017-8
(3) Karabulut, A. B., Aydin, H., Sirin, F., & Tümerdem, B. (2002). Augmentation mammaplasty by medial periareolar incision. Aesthetic plastic surgery, 26(4), 291–294. https://doi.org/10.1007/s00266-002-1339-9
(4) Hoehler, H. (1973). Breast augmentation, the axillary approach. Br J. Plast Surg 26:373.
(5) Borgognone, A., Gherardini, G., Gliosci, L., & D'Andria, D. (2017). Is periareolar incision a suitable option for breast surgery? A mathematical comparison between periareolar and inframammary fold approaches. Open Access Surgery, Volume 10, 9–14. https://doi.org/10.2147/OAS.S126714
(6) Edward M. Reece, MD, MS, Ashkan Ghavami, MD, Ronald E. Hoxworth, MD, Sergio A. Alvarez, MD, Daniel A. Hatef, MD, Spencer Brown, PhD, Rod J. Rohrich, MD, Primary Breast Augmentation Today: A Survey of Current Breast Augmentation Practice Patterns, Aesthetic Surgery Journal, Volume 29, Issue 2, March 2009, Pages 116–121, https://doi.org/10.1016/j.asj.2008.12.006
(7) ISAPS (2018) Breastfeeding after periareolar breast augmentation. Retrieved from: https://www.plasticsurgery.org/news/blog/breastfeeding-after-periareolar-breast-augmentation
(8) NHS UK. Can I breastfeed if I’m…. Retrieved from: https://www.nhs.uk/start4life/baby/feeding-your-baby/breastfeeding/can-i-breastfeed-if-im/breastfeeding-with-breast-implants/#:~:text=If%20the%20incisions%20are%20under,milk%20ducts%20have%20been%20cut.
(9) Borgognone, A., Gherardini, G., Gliosci, L., & D'Andria, D. (2017). Is periareolar incision a suitable option for breast surgery? A mathematical comparison between periareolar and inframammary fold approaches. Open Access Surgery, Volume 10, 9–14. https://doi.org/10.2147/OAS.S126714
(10) ISAPS (2018) Breastfeeding after periareolar breast augmentation: https://www.plasticsurgery.org/news/blog/breastfeeding-after-periareolar-breast-augmentation#:~:text=Does%20periareolar%20breast%20augmentation%20affect,of%20breastfeeding%20problems%20after%20surgery.
(11) Cheng, F., Dai, S., Wang, C., Zeng, S., Chen, J., & Cen, Y. (2018). Do Breast Implants Influence Breastfeeding? A Meta-Analysis of Comparative Studies. Journal of human lactation : official journal of International Lactation Consultant Association, 34(3), 424–432. https://doi.org/10.1177/0890334418776654
(12) Hyung-Bo Sim, MD, Sang-Hoon Sun, MD, Transaxillary Endoscopic Breast Augmentation With Shaped Gel Implants, Aesthetic Surgery Journal, Volume 35, Issue 8, November/December 2015, Pages 952–961, https://doi.org/10.1093/asj/sjv104
(13) Li, S., Chen, L., Liu, W. et al. Capsular Contracture Rate After Breast Augmentation with Periareolar Versus Other Two (Inframammary and Transaxillary) Incisions: A Meta-Analysis. Aesth Plast Surg 42, 32–37 (2018). https://doi.org/10.1007/s00266-017-0965-1
(14) Sevin, Asuman & Sevin, Kutlu. (2009). Breast Augmentation Using the Periareolar Approach. Breast Augmentation: Principles and Practice. 215-220. 10.1007/978-3-540-78948-2_26.
